Email: Reduce the symptoms, or treat the underlying cause?

There are different methods to help feel better and avoid problems from a hiatus hernia, such as heartburn, coughing, a lumpy feeling in the throat or swallowing difficulties. But why try something new even if medications relieve the symptoms?
We’re going to go over what you can do to get quick relief. But above all, it is important to understand how you can treat the root cause in order to be trouble-free for good.
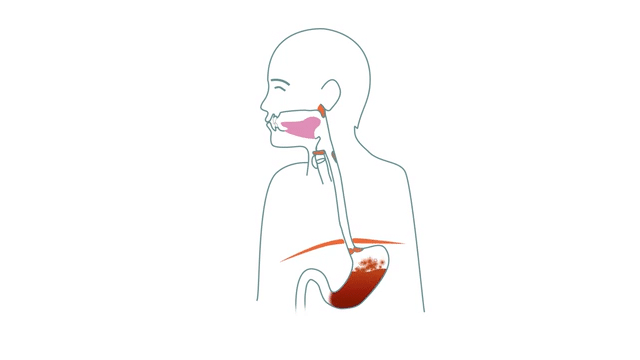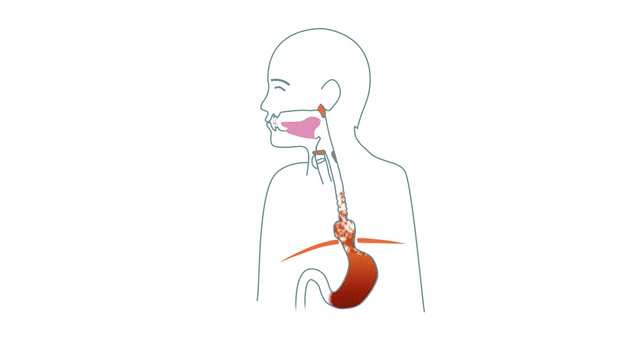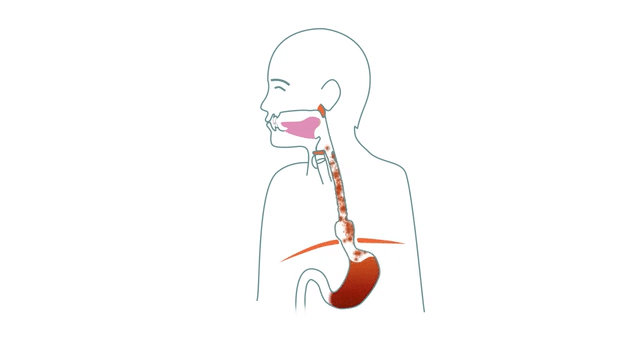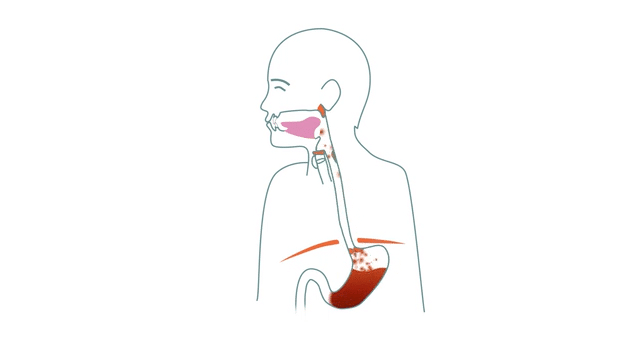
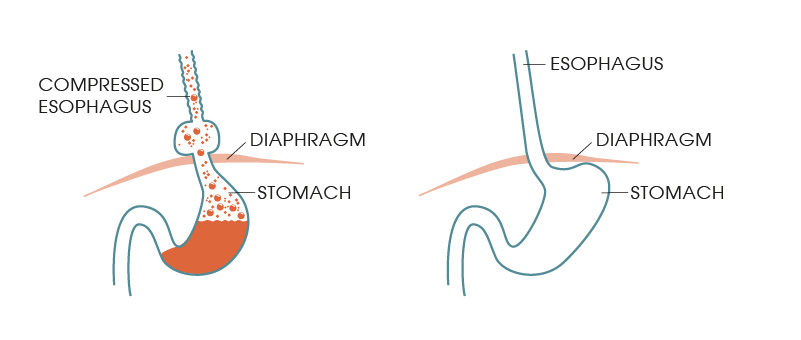
We have previously described what a hiatus hernia is and how it leads to a variety of symptoms when the stomach slides up through the diaphragm. That knowledge is important to understand the difference between different options that we are going into now. So feel free to start there if you missed it or need to go over it again.
Read more: How your problems are caused by a hiatus hernia
Symptom relief or long-term treatment?
In simple terms, there are two different ways to avoid discomfort from a hiatus hernia:
- Symptom relief that makes it feel better at temporarily, but does not do anything about the actual cause.
- Long-term treatment of the root cause that gradually reduces the problems and solves the underlying cause.
Even if you prefer to treat the root cause, it may be necessary to supplement with symptom relief to feel good before the long-term treatment has had an effect and the diaphragm has had time to be sufficiently strengthened.
Thus, there is nothing stopping you treating in the long-term and using symptom relief. But it can be problematic to only seek quick relief temporarily because the long-term treatment can take longer if you suffer with the problems for a long time.
In addition, long-term use of antacid medication can cause serious side effects and increase the risk of other diseases such as intestinal infections and pneumonia.
Short-term symptom relief
To relieve the discomfort from a hiatus hernia, you can resort to various methods:
- Home remedies
- Lifestyle changes
- Medicines
Home remedies
If you google or ask around on social media, you will get suggestions for a variety of home remedies, such as drinking bicarbonate of soda mixed with water to neutralise stomach acid, eating almonds or unsweetened lingonberry jam.
Home remedies are not something we recommend from a scientific point of view, but most are risk-free if they are taken in moderation and if they help you feel better, that’s great.
Read more: List of home remedies for heartburn and acid regurgitation
Lifestyle changes
Another way to reduce discomfort and pain is to make certain lifestyle changes. This can be losing weight, raising the head end of the bed, avoiding heavy lifting or stopping eating a number of hours before bedtime.
It is not a problem in itself to reduce discomfort and pain through different routines in everyday life. However, it can mean giving up things that are important in life such as good food, exercise and social contexts.
For many, this means that a hiatus hernia has a great impact on the entire quality of life and therefore it is important to find a long-term solution.
Antacid medicines
Common symptom relief is antacid medication, so-called PPIs (proton pump inhibitors), which about one in ten Swedes receive on prescription. This medication is good at the initial stage to reduce the corrosive impact of acid on the mucous membrane of the oesophagus. It can also be a pure necessity to cope with everyday life.
However, it is known through research that the medication is not intended for long-term consumption. At the same time, the medication also has a number of known side effects, which means that not everyone can cope with it.
If antacid medication does not help, only the worst affected people qualify for surgery, where the stomach is sewn under the diaphragm instead. Something that, in addition to relief, also entails both risks and accompanying side effects.
Today, it is possible to treat the underlying cause of the problems, which we will get into now.
Long-term treatment of the root cause
In order to be free of your symptoms in the long-term, it is important to do something about the root cause of the problems. That is, the weakened diaphragm that has lost control of the stomach, which is then allowed to slide up and down through the hole, which in turn gives a number of problems further up the muscle chain used when swallowing.
The diaphragm belongs to an important process with a total of 148 muscles that from mouth to stomach are interdependent, that they work quickly and in sync in the right order to transport food and drink down to the stomach – the swallowing process.
Learn more about the 148 muscles that work when you swallow your morning coffee.
When the diaphragm is unable to do its job, immediate problems occur in the muscular cooperation. This is when the various symptoms occur and there can also be a blockage in the oesophagus making it difficult to swallow mainly solid consistencies.
The weakened diaphragm simply needs to be strengthened again.
A simple 30-second training routine
By training with the IQoro neuromuscular training device, the root cause is treated, not just the symptoms.
The fact that it is neuromuscular means that IQoro stimulates nerves in the oral cavity that, via the brain, give commands to all the muscles in the swallowing process to start working. Even those that you normally cannot control by will.
Training is simple and does not require any contact with healthcare. The routine only takes 30 seconds and is performed three times per day for full effect. Less time than you spend brushing your teeth. Here’s how it works:
Since IQoro only uses the body’s natural system of nerve pathways and muscles, there are no negative side effects. You activate muscles from the face, lips, oral cavity, neck, all the way down into the oesophagus, diaphragm and stomach.
Initially, you may experience some muscle soreness from the exercising, which comes from muscles that you haven’t used in the same high-intensity way getting the exercise they need. This is not dangerous and quickly passes.
As time goes on, the diaphragm strengthens and your symptoms are relieved. Over time, you have treated the cause of the hernia quite naturally. By then carrying out maintenance training, you maintain the strength of the muscles so that the problems do not return.
Reduce medication in consultation with a doctor
Many people can scale back on medication, but it is important to do so in consultation with prescribing doctors because stopping medicines abruptly can have unpleasant effects.
There is no danger in using medication and exercising with IQoro at the same time. In addition, minimising unnecessary consumption of medicines is good for both health and the environment.
There is no danger in using medication and exercising with IQoro at the same time.
Even if you have had problems and perhaps taken antacids for many years, research has shown that 97 percent of people have improved statistically significantly after 6 to 8 months of training.
Improvements are noticeable gradually as the muscles are strengthened. Our customer surveys show that many people notice improvements after a few weeks into training.